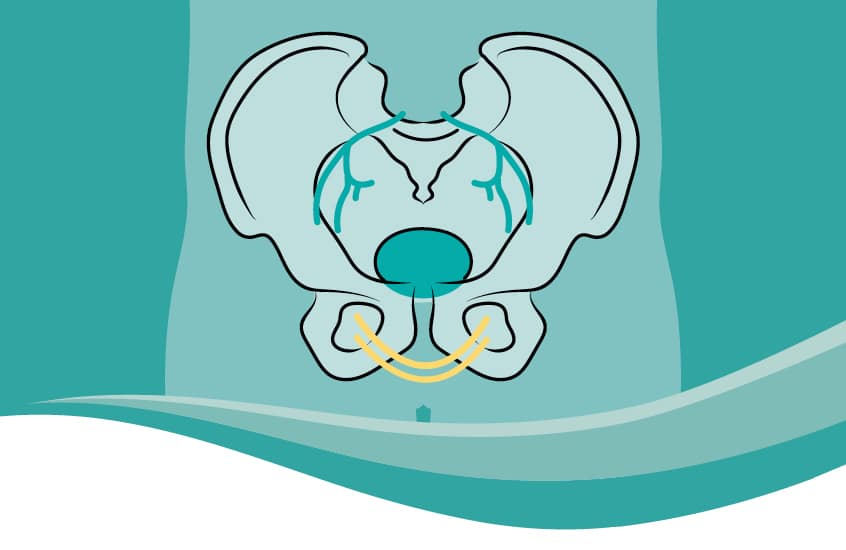
Are there risks associated with TOT?
Although serious complications are rare, there are risks to be aware of. Pre and post-procedure directions should always be followed as it helps mitigate complications.
Potential complications are:
- Bladder irritability (urgency symptoms or overactive bladder) after surgery
- Risk of damage to the vagina, bladder, urethra, or blood vessels which will require further surgery
- Risk of urinary tract infections
- Difficulty passing urine, which may require self-catheterization after the surgery usually for a few weeks
- Risk of a wound infection
- Risk of mesh becoming infected or rejected which would require the tape to be removed
- Risk of blood clots in the legs or chest
- This procedure is not aimed at improving any urgency symptoms, which are likely to persist and may deteriorate
- Small risk of tape eroding into nearby organs e.g. vagina or urethra
- Small risk of pain in groin or thigh, associated with the tape
- Risk of bleeding
What to expect pre and post-surgery?
Patients are typically admitted to the hospital the morning of their surgery, although there are occasions where they are admitted the day before. Patients are asked to bathe ahead of going in for the procedure and ensure makeup, nail varnish, and jewelry are removed. Your surgeon will discuss all other specifics ahead of the procedure including if you will be required to wear knee-length or thigh-length compression stockings.
Prior to the procedure, the anesthetist will meet with you to prepare for administering the anesthetic.
After the procedure is complete you will be cared for by nurses who will frequently check your vitals and comfort. Pain and discomfort are minimal and can be managed through pain relief medication.
A catheter and/or a vaginal pack (dressing) may be required for up to 24 hours or longer, dependent on whether any additional procedures were carried out at the same time. If a catheter is not used, you will be encouraged to urinate, and then have an ultrasound of the bladder to see if the bladder is fully emptying.
Patients are typically released the same day or day after the procedure depending on bladder function post-procedure.
Overall recovery should be fairly quick, and light activity is encouraged after 1 – 2 weeks. Passing small stitches or light vaginal bleeding and discharge can occur.
What should I do post-surgery?
- Drink 6 – 8 glasses of water per day
- Eat a balanced diet, inclusive of fresh fruits and veggies
- Keep caffeine (tea or coffee) to a maximum of 3 cups per day
- Avoid sexual intercourse or using tampons or menstrual cups for 4 – 6 weeks
- Avoid constipation
- Avoid heavy lifting (more than 30 pounds) to prevent reoccurrence of the problem
- Avoid excessive weight gain to prevent reoccurrence of the problem
- Do not smoke (it can increase the risk of failure).
To book an appointment with one of our doctors, call us at 946-2326 or email appointments@oceanmed.ky.